Liver lesions containing intracellular fat
Focal fat accumulation and diffuse fat accumulation with focal sparing
Hepatic steatosis is the result of deposition of fat in vacuoles within hepatocytes – it can be diffuse,
segmental,
or nodular.
Hepatic steatosis occurs in a number of conditions including excessive alcohol consumption,
insulin resistance,
obesity,
hyperlipidaemia,
viral infections (hepatitis B and hepatitis C) and secondary to the use of certain drugs including tamoxifen,
corticosteroids and antiretrovirals (1).
Focal fat deposition and focal sparing occur in characteristic areas including the gallbladder fossa,
in the porta hepatis and adjacent to falciform ligament or ligamentum venosum.
These patterns of focal fat accumulation and diffuse accumulation with fat sparing may mimic mass lesions (2).
Imaging findings indicative of fatty pseudolesions include the following:
- fat content
- location in areas characteristic of fat deposition or sparing (along hepatic vessels,
fissures and ligaments)
- a geographic configuration and poorly defined margins
- vessels coursing through without displacement and lack of a mass effect on other liver structures
- contrast enhancement similar to or less than that of the normal liver parenchyma (2)
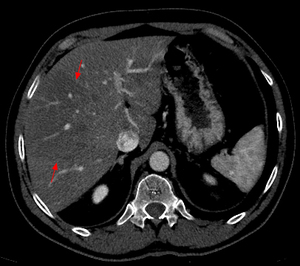
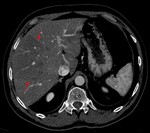
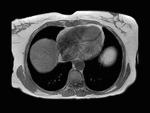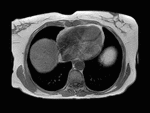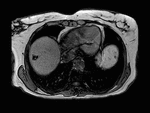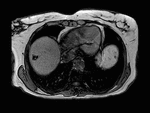
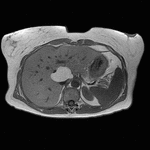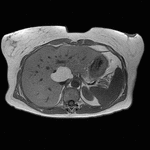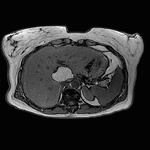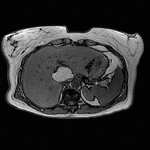
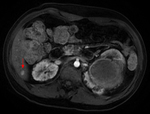
Fig. 1: Axial computed tomography image shows a large area of regional fat infiltration in segments V/VIII with a geographic appearance, lack of mass effect and preservation of the vascular architecture.
Occasionally,
varying degrees of hepatic steatosis can occur in the liver with focal hypodense areas being present in a diffusely steatotic liver on computed tomography (Figure 1).
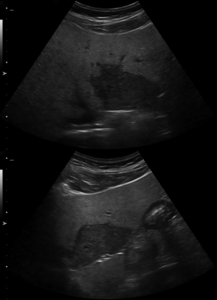
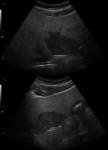
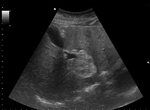
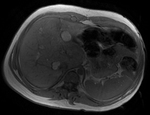
Fig. 2: Ultrasound images show features of diffuse accumulation of fat in the liver with focal fatty sparing of segment III. There is a hypoechoic area within an otherwise echogenic liver. Steatosis obscures visualisation of the intrahepatic vessels. Focal fatty sparing usually occurs in segment V of the liver or along the gallbladder fossa.
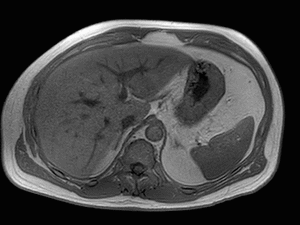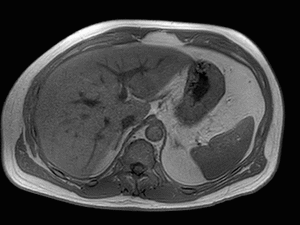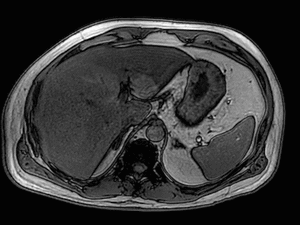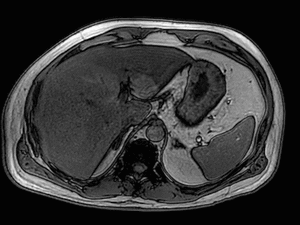
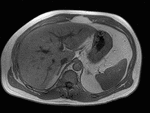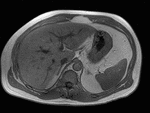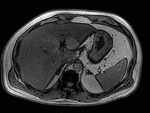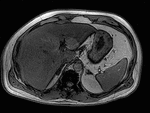
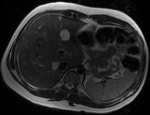
Fig. 3: Axial T1-weighted opposed-phase image demonstrates diffuse loss of signal with sparing of segment III in keeping with focal fatty sparing.
Magnetic resonance imaging plays a major role in the evaluation of focal hepatic steatosis.
Chemical shift imaging shows the presence of fat in hepatocytes by demonstrating a signal drop on opposed-phase imaging (1).
Focal hepatic steatosis appears isointense or hyperintense to the liver on in-phase T1-weighted gradient-echo imaging and there is homogenous loss of signal on opposed-phase imaging (3).
Hepatocellular carcinoma
The most common primary liver tumour in a cirrhotic liver is hepatocellular carcinoma.
Hepatocellular carcinoma,
hepatic adenoma and rarely focal nodular hyperplasia may contain microscopic fat.
Therefore,
both clinical background and imaging findings must be considered in order to reach a diagnosis (2).
Hepatocellular carcinoma demonstrates heterogeneous hypervascularity on arterial phase imaging with washout on venous and delayed phases.
Hepatocellular carcinoma may contain intracellular fat,
if it is well-differentiated.
As the grade and tumour size increase,
the intracellular fat then becomes less common and more focal in distribution (1).
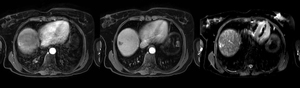
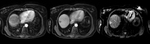
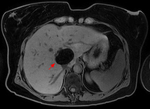
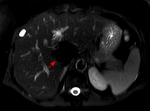
Fig. 4: Magnetic resonance images obtained in a 56-year-old lady with primary biliary cirrhosis, depict a 15 mm lesion in the subcapsular portion of segment VII which shows peripheral enhancement (left image) and venous washout (middle image). It is bright on T2-weighted imaging (right image).
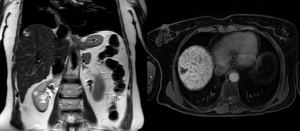
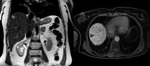
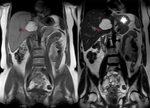
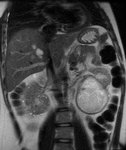
Fig. 5: Coronal T2-weighted single-shot fast spin-echo (left) image demonstrates a high signal intensity lesion in the subcapsular portion of segment VII in a 56-year-old lady with primary biliary cirrhosis.
On delayed-imaging using hepatobiliary contrast agent (right image), a hypointense focal mass is demonstrated in segment VII.
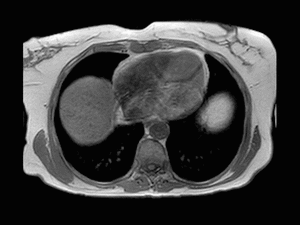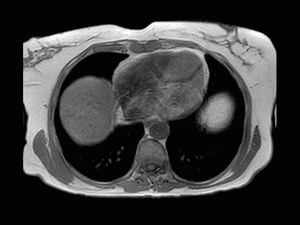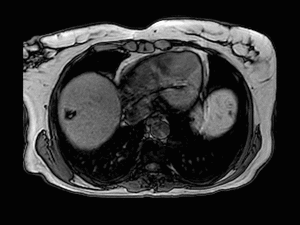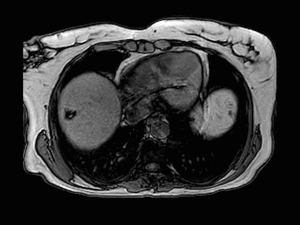
Fig. 6: Axial T1-weighted opposed-phase image shows signal intensity loss of the lesion in keeping with the presence of intracellular fat accumulation.
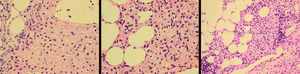
Fig. 7: Histological evaluation of the lesion in segment VII shows areas with thick hepatocyte plates, slightly enlarged hepatocytes and the presence of rather abundant fat deposition. Findings are consistent with hepatocellular carcinoma.
References: Pathology Department, Histology Section, Mater Dei Hospital -Msida/MT
Macroscopic fat-containing liver lesions
Hepatic lipoma
Hepatic lipomas are exceedingly rare benign entities,
rarer than angiomyolipomas.
Hepatic lipomas can occur sporadically (3).
Histologically lipomas are composed of mature adipose tissue.
These lesions are usually asymptomatic.
At ultrasonographic evaluation,
hepatic lipomas appear as well-circumscribed homogenously hyperechoic masses.
Hemangiomas and some hepatic metastases (gastrointestinal metastases) may also appear hyperechoic.
Hemangiomas are usually less than 3 cm in maximum dimension and metastases are usually multiple and may have a peripheral anechoic or hypoechoic halo (4).
On computed tomography and magnetic resonance imaging,
lipomas exhibit pathognomonic characteristics of a fatty mass (3).
They do not enhance after intravenous contrast administration (3).
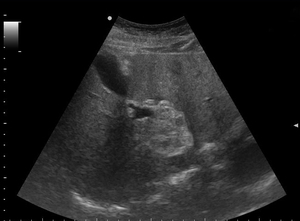
Fig. 8: Routine ultrasonography performed in a 61-year-old lady, shows a well-defined hyperechoic lesion in segment V. Further cross-sectional imaging was recommended for evaluation.
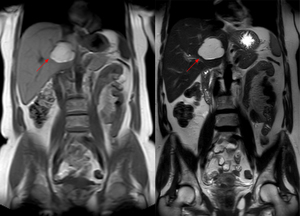
Fig. 9: On magnetic resonance, T1 (left) and T2-weighted (right) images there is a hyperintense lesion in segment V of the liver. Findings are in keeping with a hepatic lipoma.
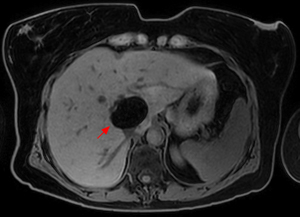
Fig. 10: Axial T1-weighted fat-suppressed image demonstrates loss of signal intensity within the lesion. Imaging findings are consistent with a diagnosis of hepatic lipoma.
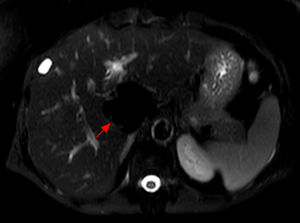
Fig. 11: Axial T2-weighted fat-suppressed image again demonstrates loss of signal within the lesion, in keeping with a hepatic lipoma.
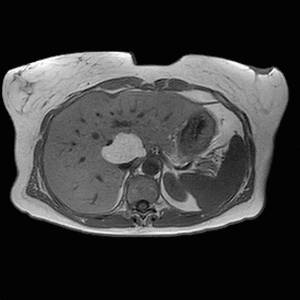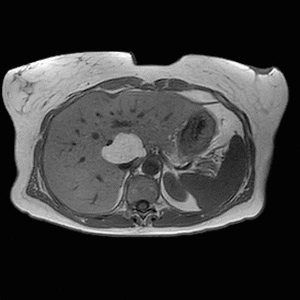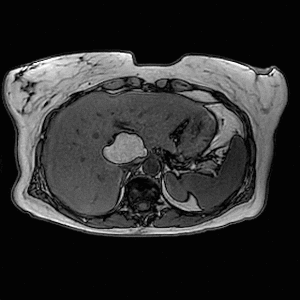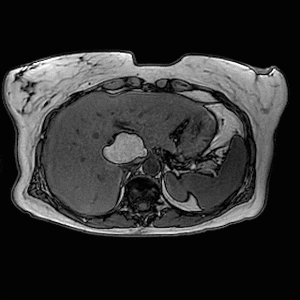
Fig. 12: Axial T1-weighted in- and opposed-phase images demonstrate loss of signal intensity within the lesion. Findings are in keeping with a hepatic lipoma.
Hepatic angiomyolipoma
This benign lesion is composed of smooth muscle cells,
thick-walled blood vessels and mature adipose tissue.
Angiomyolipomas demonstrate a variety of imaging appearances relating to the proportions of the three aforementioned components.
The amount of fat within a lesion,
can vary ranging from under 10% to over 90%.
Only 50% of hepatic angiomyolipomas contain a substantial fat content.
Hepatic angiomyolipomas are usually associated with tuberous sclerosis in 6% of cases,
as opposed to renal angiomyolipomas which are associated with tuberous sclerosis in 20% of patients (5).
On sonographic evaluation,
angiomyolipomas may be markedly echogenic,
rendering them indistinguishable from hemangiomas.
On computed tomography,
angiomyolipomas appear to consist of two components: a peripheral angiomyomatous component demonstrating soft-tissue attenuation and a fatty component (5).
Characteristically,
angiomyolipomas are non-homogeneous and the fatty component results in high signal foci on both T1-weighted and T2-weighted images.
They demonstrate a signal drop on opposed-phase images compared with in-phase images and on fat-suppressed images.
The soft tissue elements enhance with administration of intravenous contrast demonstrating the presence of vessels in and around tumours.
(1)
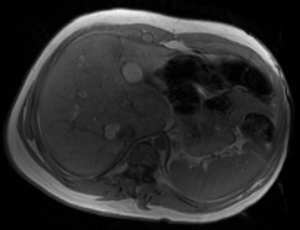
Fig. 13: Axial T1-weighted image demonstrates multiple bilobar well-defined high signal intensity lesions in a 23-year-old gentleman with tuberous sclerosis. Imaging findings are in keeping with hepatic angiomyolipomas.
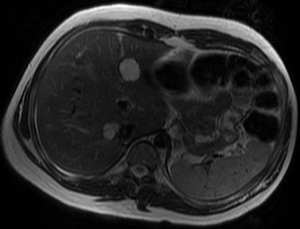
Fig. 14: Axial T2-weighted image demonstrates multiple bilobar high signal intensity lesions in a 23-year-old gentleman with tuberous sclerosis, consistent with hepatic angiomyolipomas.
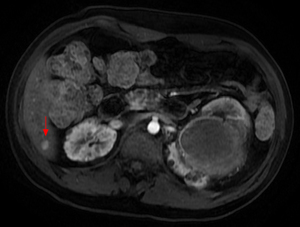
Fig. 15: Axial T1-weighted image with contrast demonstrates internal enhancement of one of the lesions in a patient with tuberous sclerosis in keeping with the presence of a hepatic angiomyolipoma.
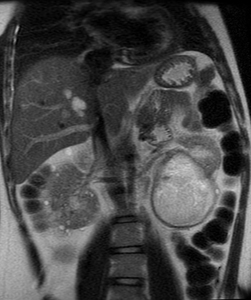
Fig. 16: Coronal T2-weighted single-shot fast spin-echo image demonstrates high signal intensity lesions within the liver of a 23-year-old gentleman with tuberous sclerosis. Both kidneys contain a large number of cysts and also fat-containing lesions in keeping with renal angiomyolipomas.
Fig. 17: Magnetic resonance T1-weighted in-phase images obtained in a 23-year-old gentleman with tuberous sclerosis demonstrate multiple fat-containing lesions within both liver lobes, the largest of which lies in segment II. Both kidneys show no normal parenchyma, a large number of cysts and fat-containing lesions in keeping with angiomyolipomas.
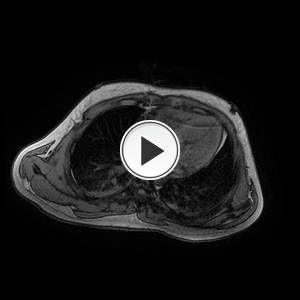
Fig. 18: Magnetic resonance T1-weighted opposed-phase images obtained in a 23-year-old gentleman with tuberous sclerosis demonstrate multiple fat-containing lesions (showing loss of signal intensity) within both liver lobes, the largest of which lies in segment II. Both kidneys show no normal parenchyma, a large number of cysts and fat-containing lesions consistent with angiomyolipomas.
Hepatic teratoma
Liver teratomas are very rare,
constituting less than one percent of all teratomas.
Hepatic teratomas have been reported more frequently in females and in most cases involve the right hepatic lobe (6).
They arise from pluripotential cells (5).
By definition,
teratomas are composed of tissue derivatives of two or more germ cell layers.
They may contain fat,
hair,
bone,
skin,
neural tissue and muscle.
The presence of a mass composed of fluid,
calcification and fat is pathognomonic of this entity (5).
Imaging findings reflect the different tissue components. Teratomas are usually discovered incidentally,
however,
sometimes acute symptoms may occur.
Teratomas are usually encapsulated lesions (6).
At ultrasonographic evaluation,
teratomas may appear anechoic or hypoechoic,
representing the cystic portion of the mass.
Hyperechoic foci may be secondary to the presence of macroscopic fat or calcification.
The fact that calcification demonstrates posterior acoustic shadowing and fat demonstrates gradual attenuation of sound,
helps to distinguish these two components (6).
At computed tomography,
macroscopic fat and calcification are easily identified as hypoattenuating and hyperattenuating components respectively.
Macroscopic fat will appear hyperintense on T1-weighted images and demonstrates signal drop out on fat-suppressed sequences (6).
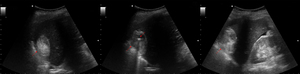
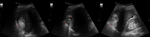
Fig. 19: Ultrasonography images obtained in a 42-year-old lady who presented to the Accident and Emergency Department with epigastric pain, show a lesion with a fat-fluid level and calcification. Fat-fluid levels secondary to the presence of sebum are considered pathognomonic of teratoma.
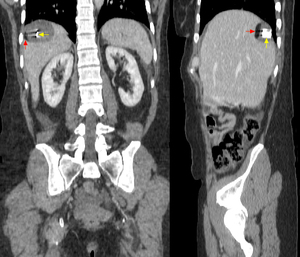
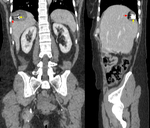
Fig. 20: Coronal (left image) and sagittal (right image) reformations demonstrate a well-defined subcapsular rounded lesion in segment VII of the liver. The lesion contains both fat and calcification consistent with a hepatic teratoma.
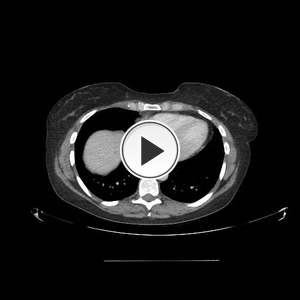
Fig. 21: Computed tomography images with contrast enhancement obtained in a 42-year-old lady who presented to the Accident and Emergency Department with epigastric pain, demonstrate an incidental finding of a well-defined lesion containing both fat and calcification in keeping with a liver teratoma. There is also evidence of acute pancreatitis.